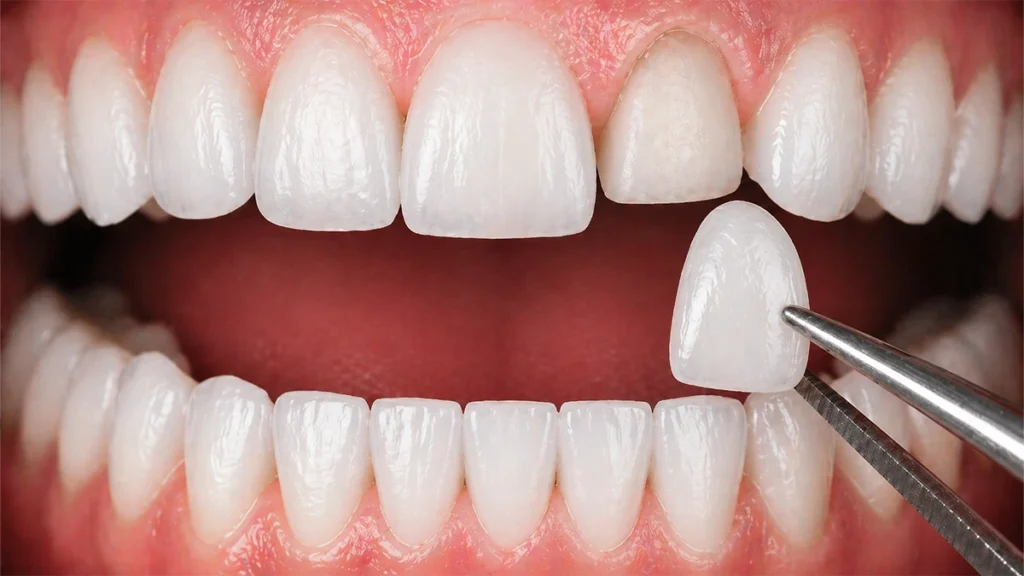
Many patients with diabetes ask: Can I safely get veneers?
In most cases, the answer is yes — but only if certain clinical conditions are met. Diabetes mellitus does not automatically prevent a person from having cosmetic dentistry, including porcelain veneers or composite veneers. However, dentists must carefully evaluate blood sugar control, gum health, infection risk, oral hygiene, and healing capacity before recommending treatment.
For diabetic patients, proper planning is essential. Stable glycemic control and healthy periodontal tissues can significantly reduce complications and support long-term veneer success.
Quick Answer: Can Diabetics Get Veneers?
Yes, many diabetic patients can get veneers safely, especially when blood sugar levels are well controlled. However, your dentist must evaluate your gum health, healing response, and overall oral condition before treatment.
In some cases, veneer treatment may be delayed until diabetes is more stable or gum disease has been treated.
Can Diabetics Get Veneers?
Diabetic patients can often receive veneers, but suitability depends on their overall oral and medical stability. Veneers are a cosmetic dental treatment placed over the front surface of teeth to improve appearance, shape, color, or minor alignment concerns.
Because veneer treatment may involve enamel preparation and close contact with the gumline, dentists need to make sure the surrounding tissues are healthy before starting.
When Veneers Are Possible with Diabetes
Veneers may be a suitable option when a diabetic patient has:
- Controlled diabetes
- Stable blood sugar levels
- Good oral hygiene
- Healthy gums
- No active infection
- No untreated periodontal disease
- Good healing response
Patients with controlled diabetes are often able to undergo cosmetic dental procedures safely. In these cases, the risk of infection, inflammation, and delayed wound healing is generally lower.
When Extra Caution Is Needed
Extra caution is needed when a patient has:
- Poor glycemic control
- Frequent hyperglycemia
- Existing gum disease
- Bleeding or swollen gums
- Poor oral hygiene
- Delayed healing history
- Active dental infection
In these situations, your dentist may recommend stabilizing your oral health first before proceeding with veneers.
Diabetes does not automatically prevent veneers. Control and stability are the most important factors.
When Diabetes May Affect Veneer Treatment
Diabetes can influence dental treatment because it affects the immune response, blood circulation, inflammation levels, and wound healing. These factors are especially important when treatment involves the gumline or enamel preparation.
Blood Sugar Control and Treatment Planning
Before veneers, your dentist may ask about your diabetes control, including your recent blood sugar levels and HbA1c result.
HbA1c gives an estimate of average blood glucose levels over the past two to three months. A higher HbA1c may suggest poor glycemic control, which can increase the risk of complications after dental treatment.
If your diabetes is not well controlled, your dentist may delay cosmetic treatment until your blood sugar levels are more stable.
Increased Risk of Infection
Diabetic patients, especially those with uncontrolled diabetes, may have a higher risk of infection. Hyperglycemia can weaken the immune response and make it harder for the body to fight bacteria.
This matters because veneer treatment must be done in a clean, healthy oral environment. If there is active gum disease, tooth decay, or infection, these problems should usually be treated first.
Delayed Healing Response
Uncontrolled diabetes can slow the body’s healing response. While veneer treatment is usually minimally invasive, some patients may experience gum irritation or sensitivity after preparation.
If blood sugar levels are unstable, healing may take longer and inflammation may be more difficult to control.
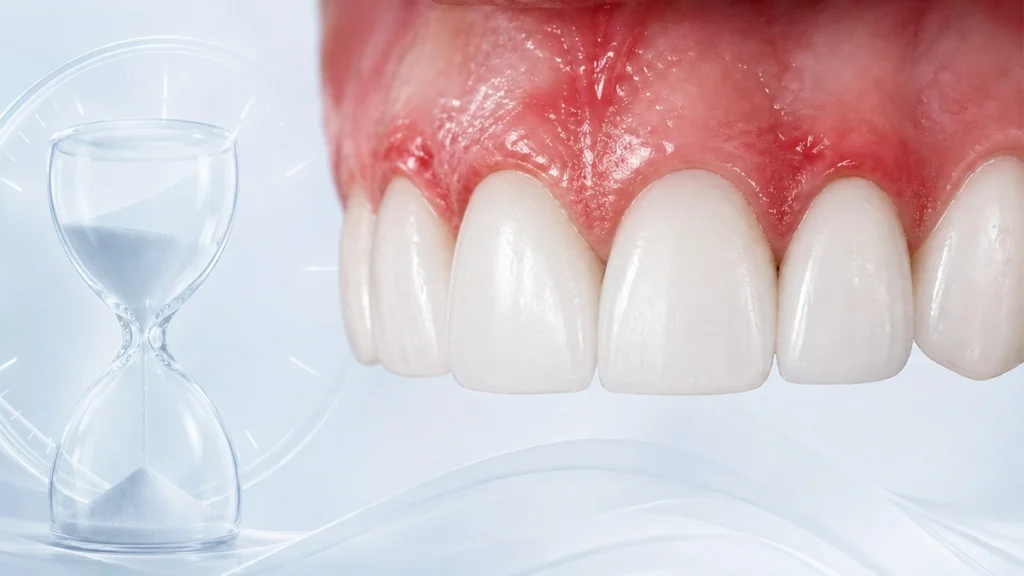
Why Gum Health Matters Before Veneers
Gum health is one of the most important factors in determining whether veneers are appropriate for diabetic patients. Even if the teeth are cosmetically suitable, unhealthy gums can compromise the final result.
Diabetes and Gum Disease
Diabetes is strongly associated with periodontal disease. Patients with diabetes may be more likely to experience gum inflammation, bleeding gums, gum recession, and bone loss around the teeth.
Periodontal disease can also make blood sugar control more difficult, creating a two-way relationship between diabetes and gum health.
Common signs of gum disease include:
- Bleeding when brushing or flossing
- Red, swollen, or tender gums
- Persistent bad breath
- Gum recession
- Loose teeth
- Deep pockets around teeth
If these signs are present, veneers should not be the first step. Gum evaluation and periodontal treatment are usually needed first.
Why Healthy Gums Are Required for Veneers
Healthy gums are essential because veneers sit close to the gumline. Inflamed or unstable gum tissue can affect how veneers fit, look, and last.
Poor gum health may lead to:
- Gum recession around veneers
- Visible veneer margins
- Inflammation around the restoration
- Higher risk of veneer failure
- Unstable cosmetic results
For long-term success, the gums must be healthy, stable, and free from active periodontal infection.
When Gum Treatment Is Needed First
If gum disease is present, your dentist may recommend periodontal therapy before veneers. This may include professional cleaning, scaling and root planing, improved home care, antibacterial treatment, or referral to a periodontist.
Once the gums are stable, veneer treatment can be reconsidered.

Does Diabetes Affect Healing After Veneer Preparation?
Diabetes can affect healing, especially when blood sugar levels are poorly controlled. However, patients with controlled diabetes often heal normally after minimally invasive dental procedures.
Healing Timeline in Diabetic Patients
For many patients, veneer preparation causes only mild temporary sensitivity or gum irritation. In controlled diabetes, this usually resolves without major concern.
In uncontrolled diabetes, healing may be slower. Gum irritation, inflammation, or sensitivity may last longer, especially if oral hygiene is poor or periodontal disease is present.
Factors That Influence Healing
Healing after veneer preparation may depend on:
- Blood sugar levels
- HbA1c control
- Gum health
- Oral hygiene
- Immune response
- Smoking status
- Existing infection
- Medication use
- Overall health
Controlled diabetes usually allows normal healing. The concern is greater when diabetes is unstable or gum disease is active.
When Veneers May Be Delayed
Sometimes, delaying veneers is the safest and most responsible clinical decision. This does not mean the patient can never have veneers. It simply means the mouth or medical condition needs to be stabilized first.
Uncontrolled Diabetes
If diabetes is poorly controlled, your dentist may recommend postponing elective cosmetic treatment. This helps reduce the risk of infection, delayed healing, and gum complications.
Active Gum Disease
Active gum disease should be treated before veneers. Placing veneers in the presence of periodontal inflammation can compromise both the health of the gums and the appearance of the final result.
Poor Oral Hygiene
Veneers require consistent maintenance. If plaque control is poor before treatment, there is a higher risk of gum inflammation, decay around veneer margins, and long-term failure.
Why Delaying Treatment Can Be Safer
Delaying veneer treatment can:
- Reduce infection risk
- Improve gum stability
- Support better healing
- Improve cosmetic results
- Increase veneer longevity
- Lower the chance of complications
A short delay for medical or periodontal stabilization may lead to a much better long-term outcome.
Read more: Who Should Get a Hollywood Smile in 2026? Candidacy, Risks, and What to Expect
Request pricing
By sending, you agree we may contact you on WhatsApp with pricing.
Got it! We’ll WhatsApp you the pricing shortly.
What Your Dentist May Ask Before Treatment
Before recommending veneers, your dentist will likely complete a detailed medical and dental evaluation. This is especially important for patients with diabetes.
Medical History and Diabetes Control
Your dentist may ask how long you have had diabetes, whether it is type 1 or type 2, and how well it is controlled.
They may also ask whether you have a history of delayed wound healing, frequent infections, or recent changes in your medical condition.
Blood Sugar Levels and HbA1c
Your dentist may ask about your recent blood glucose levels or HbA1c. In some cases, medical clearance from your physician may be recommended before elective cosmetic treatment.
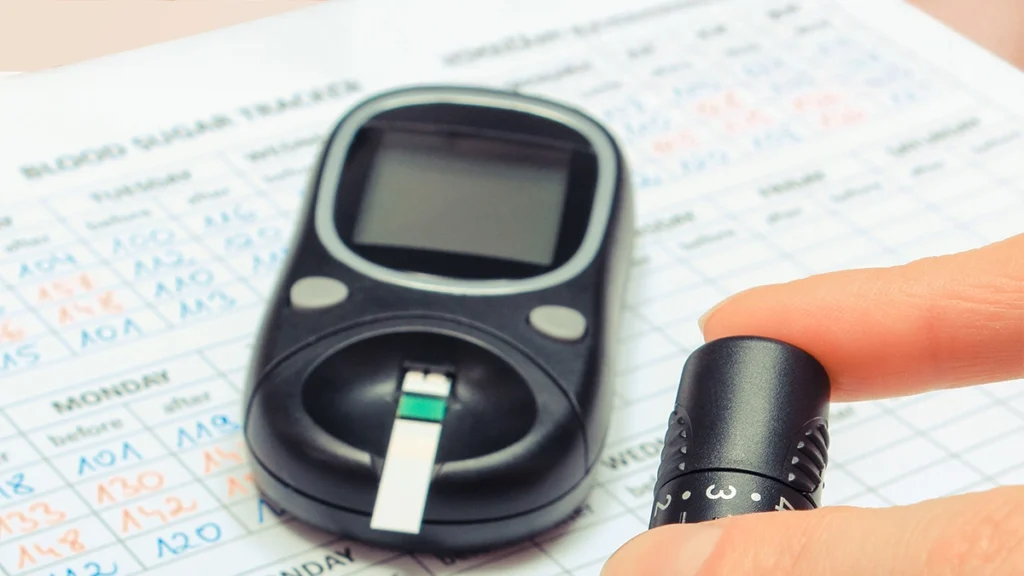
Current Medications
Your dentist should know which medications you take, including insulin, oral diabetes medications, blood pressure medications, blood thinners, or any drugs that may affect healing or bleeding.
Oral Health Examination
Your dentist will examine:
- Teeth
- Gums
- Bite alignment
- Enamel thickness
- Existing fillings or crowns
- Signs of decay
- Periodontal pockets
- Gum recession
- Plaque and tartar buildup
This examination helps determine whether veneers are safe and appropriate.
How to Prepare for Veneers If You Have Diabetes
Preparation is important for diabetic patients. The goal is to create a stable oral and medical foundation before cosmetic dentistry begins.
Maintain Stable Blood Sugar Levels
Good glycemic control supports better healing and lowers the risk of infection. Follow your physician’s diabetes management plan and keep your dentist informed of any recent changes.
Improve Your Oral Hygiene Routine
Before veneers, focus on daily plaque control. This usually includes brushing twice daily, flossing or using interdental cleaners, and attending professional dental cleanings as recommended.
Treat Any Gum Issues First
If you have bleeding gums, swelling, or periodontal disease, these issues should be treated before veneer placement.
Pre-Treatment Checklist
Before getting veneers, diabetic patients may benefit from:
- Recent dental examination
- Recent professional cleaning
- Periodontal evaluation
- Stable blood sugar control
- Recent HbA1c information
- Medical clearance if needed
- Good daily oral hygiene
- No active gum infection
- No untreated tooth decay
Read more: How a Hollywood Smile Is Planned Safely in Turkey in 2026: What Dentists Check Before Treatment
Request pricing
By sending, you agree we may contact you on WhatsApp with pricing.
Got it! We’ll WhatsApp you the pricing shortly.
Are Veneers the Best Option or Is Another Treatment Better?
Veneers can be an excellent cosmetic treatment, but they are not always the best option for every patient. Your dentist will recommend treatment based on your oral health, tooth structure, cosmetic goals, and diabetes stability.
When Veneers Are Suitable
Veneers may be suitable for improving:
- Tooth discoloration
- Minor chips
- Small gaps
- Uneven tooth shape
- Mild cosmetic misalignment
- Worn tooth edges
- Smile symmetry
They are best used when teeth are structurally healthy and the gums are stable.
Alternative Treatments
Depending on your condition, your dentist may recommend another treatment instead of veneers.
Teeth Whitening
If the main concern is tooth color, professional whitening may be a more conservative option than veneers.
Crowns
If a tooth has significant structural damage, large fillings, cracks, or severe wear, a crown may be more appropriate than a veneer.
Orthodontic Options
If alignment or spacing is the main issue, orthodontic treatment may provide a better long-term solution.
Read more: Veneers vs Whitening: Which Treatment Actually Changes Your Smile?
Risks and Considerations for Diabetic Patients
For diabetic patients, veneer treatment requires careful planning because certain risks may be higher when diabetes is not well controlled.
Infection Risk
Uncontrolled diabetes may increase infection risk due to reduced immune response and impaired healing.
Gum Inflammation
Diabetes can increase susceptibility to gum inflammation and periodontal disease. This may affect how veneers look and function over time.
Healing Variability
Healing response can vary between patients. Controlled diabetes usually allows predictable healing, while uncontrolled diabetes may cause slower or less predictable recovery.
Veneers in Diabetic Patients — Risk Overview
| Factor | Controlled Diabetes | Uncontrolled Diabetes |
| Healing | Usually normal | May be slower |
| Infection risk | Lower | Higher |
| Gum health | Often stable with good care | Often more compromised |
| Treatment eligibility | Usually suitable after evaluation | May require delay |
| Long-term veneer success | More predictable | Less predictable if gums are unstable |
| Need for medical review | Sometimes | More likely |
When to Book a Consultation
A consultation is the best way to determine whether veneers are safe for you. Your dentist can evaluate your diabetes status, gum health, bite, enamel, and cosmetic goals.
Signs You May Be Ready
You may be a good candidate for veneers if:
- Your diabetes is stable
- Your blood sugar is well controlled
- Your gums are healthy
- You do not have active gum disease
- Your oral hygiene is consistent
- Your teeth are structurally suitable
Signs You Should Wait
It may be better to delay veneers if you have:
- Bleeding gums
- Swollen gums
- Poor blood sugar control
- Active infection
- Untreated tooth decay
- Poor oral hygiene
- Recent uncontrolled hyperglycemia
- A history of delayed healing
Which treatment are you interested in?
People Also Ask About Veneers and Diabetes
Can diabetics get veneers safely?
Yes, diabetic patients can often get veneers safely if their diabetes is controlled and their gums are healthy. A dental evaluation is necessary before treatment.
Do veneers heal slower in diabetic patients?
Healing may be slower if diabetes is poorly controlled. Patients with stable blood sugar levels usually heal normally after veneer preparation.
Are veneers safe with diabetes?
Veneers can be safe for people with diabetes when there is good glycemic control, healthy gums, and no active infection.
Can diabetics get porcelain veneers?
Yes, diabetic patients can get porcelain veneers if their oral health is stable and their dentist confirms they are suitable candidates.
Should gum disease be treated before veneers?
Yes. Gum disease should be treated before veneers because inflamed or unstable gums can affect healing, veneer fit, appearance, and long-term success.
Final Insight — Diabetes Does Not Exclude You from Veneers
Diabetes does not automatically prevent you from getting veneers. What matters most is control, stability, and oral health.
Patients with well-controlled diabetes and healthy gums are often good candidates for veneers. However, uncontrolled diabetes, active gum disease, or poor oral hygiene may require treatment delay.
The safest approach is to have a full dental evaluation before beginning cosmetic dentistry. With proper planning, stable blood sugar levels, and healthy periodontal tissues, veneers may be a safe and successful option for many diabetic patients.
Read more: What Are Dental Veneers? Types, Uses, and Who They Are For
FAQ
Yes. You can get veneers if you have diabetes, provided your blood sugar is well controlled and your gums are healthy.
Healing may be slower in diabetic patients if diabetes is not well controlled. With stable glycemic control, healing is usually normal.
Yes. Veneers are generally safe for people with controlled diabetes after proper medical and dental evaluation.
Yes. Diabetic patients can get porcelain veneers if their oral health is stable and there is no active gum disease or infection.
Yes. Gum disease should always be treated before veneers to reduce inflammation, improve stability, and support long-term results.
Yes. High blood sugar may increase inflammation, infection risk, and delayed healing, which can affect veneer treatment outcomes.
Diabetes itself does not necessarily cause veneer failure. However, uncontrolled diabetes, gum disease, and poor oral hygiene can increase the risk of complications.
Yes. Always tell your dentist if you have diabetes, what medications you take, and whether your blood sugar is well controlled. This helps your dentist plan treatment safely.