Many patients considering veneers ask an important question:
Can I safely get veneers if I have a medical condition?
In many cases, the answer is yes — but treatment planning must be personalized. Dentists evaluate overall health, medications, gum condition, and healing ability before recommending veneers. Understanding how medical conditions interact with cosmetic dentistry is essential for safe and predictable results.
Quick Answer: Can Patients With Medical Conditions Get Veneers?
Yes, many patients with medical conditions can safely get veneers, especially when their condition is well managed. However, dentists must evaluate factors such as blood sugar control, blood pressure, medications, gum health, and healing response before proceeding. In some cases, treatment may require precautions or be delayed until the patient is stable.
What Dentists Evaluate Before Placing Veneers
Before placing veneers, a dentist should complete a full clinical assessment. Veneers are cosmetic restorations, but they still involve biological tissues, tooth structure, gum health, and sometimes local anesthesia. For patients with medical conditions, this evaluation becomes even more important.
Medical History and Current Health Status
Dentists need to understand the patient’s general health before starting treatment. This includes both chronic diseases and recent medical events.
Important medical history may include:
- Diabetes mellitus
- Hypertension
- Heart disease
- Bleeding disorders
- Autoimmune diseases
- Immune suppression
- Previous stroke or heart attack
A patient with a medical condition may still be suitable for veneers, but the condition must be stable enough for elective cosmetic treatment.
For example, a patient with well-controlled diabetes may often proceed safely, while a patient with uncontrolled blood glucose levels may need medical stabilization before treatment.
Medications and Their Effects
Medication review is a critical part of veneer planning. Some medications can affect bleeding, healing, oral dryness, gum condition, or infection risk.
Dentists commonly ask about:
- Blood thinners
- Antiplatelet medications
- Steroids
- Immunosuppressive medications
- Blood pressure medication
- Diabetes medication
Patients should never stop or change prescribed medication without medical advice. If a medication affects dental treatment, the dentist may coordinate with the patient’s physician to decide whether any precautions are needed.
Gum Health and Oral Condition
Veneers require more than cosmetically suitable teeth. They also need a stable and healthy oral foundation. Before recommending veneers, the dentist will carefully assess the gums, teeth, enamel, bite, and overall oral hygiene.
During the clinical evaluation, the dentist may assess:
- Periodontal health and gum inflammation
- Bleeding on probing
- Plaque and calculus buildup
- Gum recession
- Tooth mobility
- Enamel thickness
- Existing fillings, crowns, decay, or damaged tooth structure
- Bite pressure and signs of grinding or clenching
If active gum disease, significant inflammation, untreated decay, or poor oral hygiene is present, these issues usually need to be treated before veneers are placed. This helps create a healthier foundation and improves the chances of achieving a stable, natural-looking, and long-lasting result.
Why Medical Evaluation Is Critical Before Cosmetic Dentistry
Medical evaluation helps prevent avoidable complications. Veneers are often considered an aesthetic treatment, but the procedure still interacts with living tissues.
A proper medical and dental assessment can help:
- Reduce bleeding risk
- Lower infection risk
- Improve healing
- Protect gum health
- Improve veneer bonding success
- Avoid unnecessary treatment delays
- Support long-term veneer stability
- Identify safer alternatives when needed
A safe cosmetic plan is not only about creating a beautiful smile. It is about creating a smile that is biologically appropriate for the patient.

Are Veneers Safe for Patients With Chronic Conditions?
Many patients with chronic conditions can get veneers safely. This includes patients with controlled diabetes, stable high blood pressure, well-managed autoimmune disease, and many cardiovascular conditions.
When Veneers Are Generally Safe
Veneers are generally safer when the patient has:
- Stable medical health
- Controlled chronic conditions
- Good oral hygiene
- Healthy gums
- No active oral infection
- No uncontrolled bleeding risk
- Realistic expectations
- Adequate enamel for bonding
- No severe untreated grinding habit
A patient with a chronic condition may still be a good candidate for veneers if the condition is well managed and does not significantly interfere with healing, infection control, or dental treatment safety.
When Extra Precautions Are Needed
Extra precautions may be needed when a patient has:
- Poorly controlled diabetes
- Unstable blood pressure
- Recent cardiovascular events
- Active autoimmune disease flare-ups
- Bleeding disorders
- Immunosuppression
- Severe gum inflammation
- Multiple medications affecting healing
- High anxiety or stress response during dental treatment
In these cases, the dentist may request medical clearance, adjust appointment length, monitor vital signs, or delay treatment until the patient is more stable.
Safety depends more on stability than diagnosis. A controlled medical condition is often less concerning than an undiagnosed or poorly managed one.
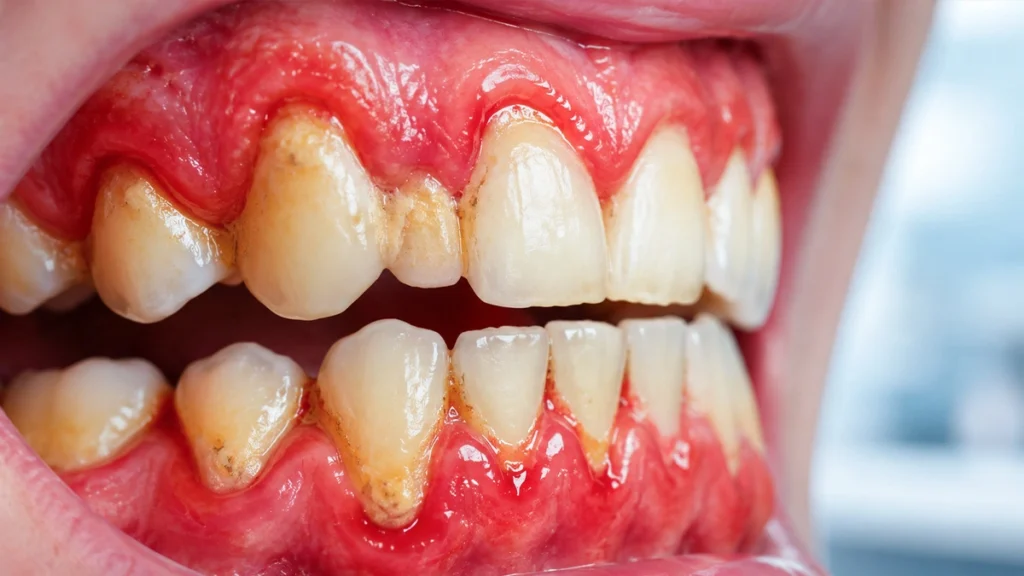
Can Diabetics Get Veneers?
Yes, many people with diabetes can get veneers, but blood sugar control is very important.
Diabetes mellitus can affect oral health, especially the gums. The ADA notes that diabetes can cause oral changes involving the gums, saliva, taste, and breath, while the CDC states that gum disease is more common in people with diabetes.
Impact of Blood Sugar Control
Poor glycemic control can increase the risk of gum inflammation, infection, dry mouth, and delayed healing. These factors may affect veneer preparation, gum response, and long-term maintenance.
Before veneers, the dentist may ask about HbA1c levels, recent blood sugar stability, diabetes medications, and history of infections or slow healing.
Healing and Infection Risk
Veneer treatment is usually less invasive than dental implants or extractions, but the gums may still be affected during preparation, impressions, temporary veneers, and cementation. If the gums are inflamed or healing is poor, the final result may be less predictable.
When Diabetes Requires Treatment Delay
Veneer treatment may be delayed if diabetes is uncontrolled, gum disease is active, there are signs of infection, or the patient has a history of poor wound healing. Delaying treatment allows the dentist and physician to reduce risk and improve cosmetic outcomes.
Read more: Can Diabetics Get Veneers? What to Know Before Cosmetic Dentistry
Can People With High Blood Pressure Get Veneers?
Yes, patients with high blood pressure can often receive veneers if their blood pressure is stable and monitored.
Hypertension is one of the most common chronic cardiovascular conditions, and the ADA highlights blood pressure measurement as an important screening vital sign during dental visits.
Blood Pressure Stability and Safety
Dental treatment can cause stress, and stress may temporarily raise blood pressure. For this reason, dentists may check blood pressure before treatment, especially if the patient has known hypertension or cardiovascular risk.
Stress and Dental Procedures
Patients with dental anxiety may benefit from shorter appointments, calm communication, local anesthesia when needed, and careful pain control. Reducing stress can make veneer treatment safer and more comfortable.
When Monitoring Is Required
Monitoring may be needed if the patient has very high blood pressure, recent medication changes, chest pain history, heart disease, or previous cardiovascular events. In some cases, medical clearance may be recommended before starting treatment.
Read more: Can People With High Blood Pressure Get Veneers? Dentist Guidance Before Treatment
Request pricing
By sending, you agree we may contact you on WhatsApp with pricing.
Got it! We’ll WhatsApp you the pricing shortly.
Other Medical Conditions That May Affect Veneer Treatment
Veneers are not only affected by diabetes or hypertension. Several other medical conditions can influence treatment planning.
Cardiovascular Conditions
Patients with heart disease, previous heart surgery, valve problems, stroke history, or implanted cardiac devices may need a more detailed medical review. The dentist may adjust appointment length, anesthesia choices, and stress-control measures.
Autoimmune Diseases
Autoimmune diseases such as rheumatoid arthritis, lupus, Sjögren’s syndrome, or inflammatory bowel disease may affect oral dryness, gum health, inflammation, or healing. Some medications used for autoimmune conditions may also influence immune response.
Bleeding Disorders
Patients with clotting disorders, low platelet counts, or anticoagulant therapy require careful planning. Veneer preparation itself may not cause heavy bleeding, but gum work, impressions, retraction cords, or contouring can irritate soft tissue.
Immunocompromised Patients
Patients undergoing chemotherapy, organ transplant therapy, high-dose steroids, or immune-suppressing treatment may have higher infection risk. Dental treatment should be coordinated carefully, and elective cosmetic care may need to wait until the patient is medically stable.
Why Each Condition Requires Individual Assessment
Two patients with the same diagnosis may have very different risk levels. A patient with well-controlled diabetes may be a better veneer candidate than a patient with untreated gum disease and no systemic diagnosis. This is why dentists assess the whole patient, not only the smile.
Medical Conditions That May Affect Healing or Treatment Planning
Some conditions do not prevent veneers but may change how treatment is performed.
Delayed Healing Conditions
Diabetes, immune disorders, nutritional deficiencies, smoking, and some medications can slow tissue healing. If gums do not heal well, veneer margins may become irritated or exposed.
Increased Infection Risk
Poorly controlled blood sugar, active gum disease, immune suppression, and poor oral hygiene can increase infection risk. Dentists usually prefer to treat inflammation before beginning cosmetic work.
Medication Interactions
Some medications may interact with dental anesthetics, antibiotics, pain relievers, or anti-inflammatory drugs. Patients should bring a complete medication list to the consultation.
How Dentists Adjust Treatment Plans
Dentists may recommend medical clearance, periodontal treatment first, digital smile design, minimally invasive veneers, shorter visits, gentler gum management, or longer healing time between appointments.
When Veneers May Require Extra Precautions
Some patients can proceed with veneers, but only with added precautions.
Pre-Treatment Stabilization
Before veneers, the dentist may recommend that the patient stabilize their condition first. This may include:
- Improving blood sugar control
- Managing blood pressure
- Treating gum inflammation
- Completing dental cleaning
- Managing dry mouth
- Treating active cavities
- Reviewing medications with a physician
Stabilization improves the chance of a safe and successful outcome.
Shorter Appointments
Shorter appointments may be helpful for patients with:
- High blood pressure
- Dental anxiety
- Cardiovascular conditions
- Fatigue-related medical conditions
- Difficulty sitting for long periods
- Pain sensitivity
Breaking treatment into smaller steps can reduce stress and improve patient comfort.
Medical Clearance
Medical clearance may be recommended when the dentist needs additional information about the patient’s health status or treatment risk.
This may be important for patients with:
- Recent heart attack or stroke
- Uncontrolled diabetes
- Significant bleeding risk
- Immune suppression
- Complex medication use
- Serious systemic disease
- Recent surgery or hospitalization
Medical clearance helps the dentist plan treatment safely, but it does not replace the dentist’s own clinical evaluation.
Monitoring During Treatment
Some patients may require monitoring during dental procedures. This may include checking:
- Blood pressure
- Heart rate
- Symptoms of dizziness or anxiety
- Signs of bleeding
- Gum response
- Pain or sensitivity
Monitoring helps identify problems early and supports safer treatment.
Read more: What Are Dental Veneers? Types, Uses, and Who They Are For
When Veneers May Need to Be Delayed
Sometimes delaying treatment is the safest decision.
Uncontrolled Medical Conditions
Veneers may need to wait if a medical condition is unstable. Examples include uncontrolled diabetes, very high blood pressure, active infection, recent heart attack, recent stroke, or ongoing cancer therapy.
Active Gum Disease
Active periodontal disease must be treated before veneers. Veneers placed on inflamed gums are more likely to cause discomfort, bleeding, poor margins, and aesthetic failure.
High Risk of Complications
If healing is poor, infection risk is high, or medications cannot be safely managed, the dentist may recommend delaying veneers or choosing a less invasive cosmetic option.
Why Delaying Can Improve Outcomes
Delaying treatment is not a failure. It can improve safety, gum stability, veneer fit, color matching, and long-term success.
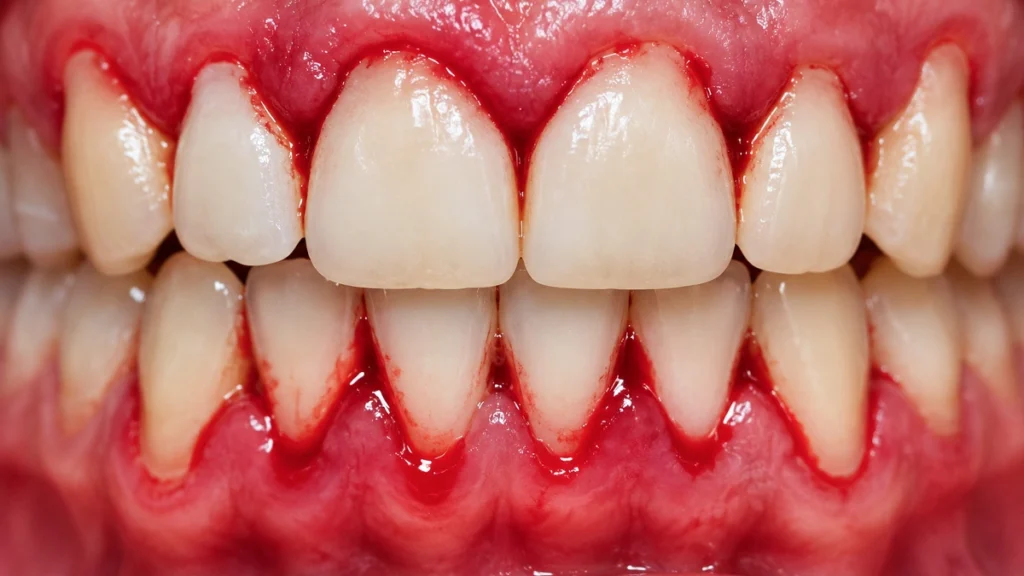
Who Is a Good Candidate for Veneers With Medical Conditions?
A good candidate for veneers is not necessarily someone with perfect health. A good candidate is someone whose health and oral condition are stable enough for treatment.
Stable Health Status
Patients with controlled chronic conditions are often suitable candidates. The dentist may ask for recent medical updates, physician input, or laboratory results when needed.
Good Oral Hygiene
Veneers require daily brushing, flossing, and regular dental checkups. Patients with poor oral hygiene may develop gum inflammation or decay around veneer margins.
Controlled Risk Factors
Good candidates usually have controlled blood sugar, stable blood pressure, healthy gums, no active infection, and realistic expectations.
When a Patient May Not Be a Candidate
A patient may not be a good candidate for veneers if they have uncontrolled disease, active gum disease, severe enamel loss, untreated decay, heavy teeth grinding, or unrealistic expectations.
Read more: Veneers in Turkey: Before & After, Prices, and Procedure Explained
Questions to Ask Your Dentist Before Veneers
Before starting veneer treatment, medically sensitive patients should ask:
Is my condition stable enough for treatment?
Your dentist should explain whether your current health status is suitable for veneers or whether treatment should wait.
Do my medications affect the procedure?
Bring a full medication list, including blood thinners, immune medications, diabetes medication, steroids, and supplements.
Are there safer alternatives?
In some cases, whitening, bonding, orthodontics, or gum treatment may be safer or more conservative than veneers.
What precautions will be taken?
Ask whether you need blood pressure monitoring, medical clearance, shorter appointments, periodontal treatment, or special aftercare.
How to Prepare for Veneers If You Have a Medical Condition
Preparation can reduce risk and improve results.
Manage Your Condition First
Follow your physician’s advice, take medications as prescribed, and avoid starting cosmetic treatment during unstable medical periods.
Follow Medical Advice
Do not stop blood thinners, diabetes medication, blood pressure medication, or immune therapy without medical guidance.
Improve Oral Hygiene
Brush twice daily, clean between the teeth, and treat gum inflammation before veneers. Healthy gums help veneers look natural and last longer.
Pre-Treatment Checklist
Before veneers, patients may need:
- Medical consultation if the condition is complex.
- Dental cleaning and gum evaluation.
- Medication review.
- Blood pressure check.
- Diabetes control review when relevant.
- Treatment plan discussion.
- Clear follow-up instructions.
Read more: Dental Tourism in Turkey: What You Need to Know Before Booking
Veneers vs Other Cosmetic Options for Medically Sensitive Patients
Veneers are not the only cosmetic dentistry option. The safest choice depends on oral health, enamel condition, medical stability, and aesthetic goals.
When Veneers Are Suitable
Veneers may be suitable for discoloration, minor shape issues, small gaps, worn edges, or mild alignment concerns when the teeth and gums are healthy.
When Alternatives Are Better
Alternatives may be better when the patient needs a more conservative, reversible, or lower-risk approach.
Teeth Whitening
Whitening may be suitable for natural tooth discoloration when enamel is healthy and no major shape correction is needed.
Composite Bonding
Composite bonding may be useful for small chips, gaps, or shape changes. It is usually more conservative than porcelain veneers.
Crowns
Crowns may be needed when teeth are heavily damaged, weakened, cracked, or previously restored. However, crowns are more invasive than veneers and require careful planning.
People Also Ask About Veneers and Medical Conditions
- Can patients with medical conditions get veneers?
- Are veneers safe with chronic illness?
- Do medical conditions affect cosmetic dentistry?
- Can medications affect veneer treatment?
- Who is not a good candidate for veneers?
Final Insight: Medical Conditions Do Not Automatically Exclude You
Having a medical condition does not automatically mean you cannot get veneers. In many cases, safe treatment is possible with proper planning.
The most important factor is stability. A controlled medical condition is often easier to manage than untreated gum disease, poor oral hygiene, or hidden infection.
For patients considering veneers in Turkey in 2026, the safest approach is to choose an authorized clinic, share your complete medical history, disclose all medications, and allow the dentist to coordinate with your physician when needed.
With careful evaluation, personalized planning, and realistic expectations, many medically sensitive patients can achieve a healthier, more confident smile safely.
Which treatment are you interested in?
FAQ
Yes. Many patients can get veneers if their condition is stable and properly evaluated by a dentist.
They can be safe when precautions are taken and the treatment plan is individualized.
Yes. Some medications may influence bleeding, healing, dry mouth, infection risk, or procedure planning.
Patients with uncontrolled medical conditions, active oral disease, untreated decay, severe gum inflammation, or high complication risk may need to delay treatment.
In some cases, yes. Medical clearance may be recommended for patients with complex medical conditions, immune suppression, bleeding risk, or unstable chronic disease.